Skipped Cancer Screenings: Racial Inequality, Coronavirus, or Denial?
As the nation moves towards a new era of inclusivity and diversity, the American Society of Clinical Oncology (ASCO)’s fourth annual survey sheds light on racial inequality and other issues that influence cancer screening and health care access amidst the COVID-19 pandemic.
ASCO’s National Cancer Opinion Survey is a largely accessible national representative survey conducted by The Harris Poll. The 2020 survey, conducted virtually from July 21st to September 8th, revealed that 4,012 U.S. adults aged 18 and older are suffering or have suffered from cancer in 2020 alone. ASCO President Lori Pierce, MD, FASTRO, FASCO said that “this survey assesses Americans’ perceptions of a wide range of cancer prevention and care issues during a most turbulent time in our country,” with the goal of addressing these needs within the context of access to cancer screening.
In line with the national racial equality crisis, and the Black Lives Matter Movement, this year’s survey placed a focus on understanding whether race can affect health care access. The survey found that 59% of Americans are aware of racial disparities impacting the care a person receives, with a majority of these views belonging to those in racial and ethnic minorities.
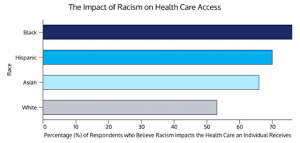
Figure 1: The Impact of Racism on Health Care Access. ASCO’s National Cancer Opinion Survey found that the majority of racial minorities (including Blacks, Hispanics, and Asians) argue that racism impacts the care an individual receives.
71% of respondents belonging to the Black ethnic group believe that they are less likely to receive the same quality of cancer care as Caucasians, while only 47% of Caucasians seem to agree with this belief. This large divide between the opinions of the two groups potentially stems from the fact that Caucasians aren’t overtly subjected to racial discrimination when it comes to their health care rights and quality of care, and they may subconsciously choose to believe that it does not exist. It could also be due to the lack of adequate information surrounding the extent of racial disparities within health care. This unconscious ignorance seen within the large majority of the American population needs to be resolved so that the nation can move forward to incorporate racial equality in cancer health care access.
Another prominent issue that ASCO has raised is the unequal distribution of good health care insurance within the population—56% of Americans argue that the type of health care insurance influences the likelihood of cancer survival. Additionally, despite increasing evidence showing worsened cancer prognosis in racial minorities, particularly for those belonging to the Black minority, fewer than 1 in 5 (19%) Americans actively believe that race impacts cancer survival, with Hispanic and Black respondents holding these views more than Whites. Dr. Pierce argues that “racism undermines public health,” significantly affecting those suffering from cancer. She also states that “for almost every cancer, Black Americans fare worse than other racial groups” and that “now is the time to address the systemic issue of health inequity that negatively impact the health of Blacks and other people of color.”
Another surprising discovery from 2020’s National Cancer Opinion Survey is that a hefty two-thirds of Americans have either delayed or avoided their cancer screenings due to fear surrounding the COVID-19 pandemic. While pushing cancer screenings for a couple of months is not necessarily life-threatening, ASCO’s Chief Medical Officer Richard L. Schilsky, MD, FACP, FSCT, FASCO, is concerned that “a significant number of Americans might stop getting preventative care for long periods of time or altogether,” inevitably causing a drastic surge in cancer-associated morbidity and mortality. Though screenings may seem subjectively avoidable during a global pandemic, cancer can be well managed through screening—data shows that a majority of cancer-related deaths could be prevented with early screening and diagnostic measures.
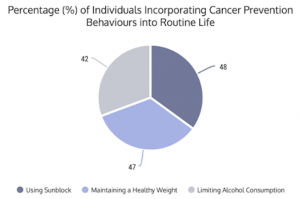
Figure 2: Incorporation of Cancer Prevention Behaviors into Routine life. The National Cancer Opinion Survey conducted by ASCO consistently reports that a large proportion of the population do not include cancer prevention behaviors (usage of sunblock, healthy weight, and limited alcohol consumption) into their daily schedules.
Simultaneous to increased delays in cancer screenings, previous ASCO National Cancer Opinion surveys have also reported that most Americans are not incorporating cancer prevention behaviors into their regular schedules. For instance, less than half of the respondents use sunblock, maintain a healthy weight, or limit alcohol consumption, thereby increasing their cancer risk. While these cancer prevention steps may not seem that important in light of the current global situation, they are vital to reducing an individual’s risk of developing cancer. Therefore, researchers, oncologists, medical doctors, and other health care professionals strongly recommend incorporating these behaviors into daily routines.
To conclude, this year’s National Cancer Opinion Survey conducted by ASCO uncovers several issues within the American health care system, namely unequal access to cancer screenings due to racial disparities, cancer screening denial, and fear of developing COVID-19. In light of recent events and unprecedented circumstances, researchers and health care professionals now more than ever argue that it is imperative to proactively find solutions to these issues to better transform the future of the American health care system.


Leave a Reply
Want to join the discussion?Feel free to contribute!